This is a Quick Tips post providing a basic answer to a commonly asked question often faced within the field of archaeology and anthropology.
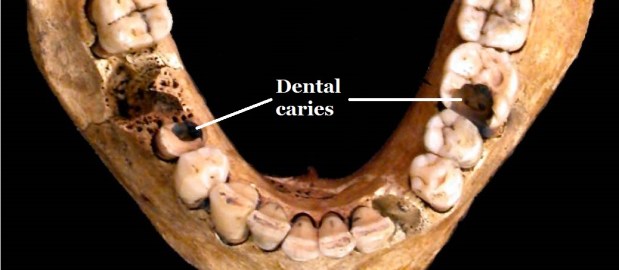
Some diseases are more easily to identify on skeletal remains due to leaving tell-tale signs in the bones preservation. An easy example of this is osteoporosis; this condition leaves the inners of bones a lot more porous which is easier to visually assess and compare to a ‘healthy’ individual’s skeletal remains.

Some diseases are more easily to identify on skeletal remains due to leaving tell-tale signs in the bones preservation. An example of this is osteoporosis; this condition leaves the inners of bones a lot more porous than normal bones.
A study by Hershkovitz & Rothschild (1997) highlighted how certain medical conditions, in their study sickle cell anaemia, affects the bone growth and development. Hershkovitz & Rothschild found that due to the iron deficiency from sickle cell anaemia caused porotic hyperostosis (symmetrical osteoporosis) on the parietal bone as well as others. They were able to visually diagnose this due to the characteristic ‘pores’ over the skull.
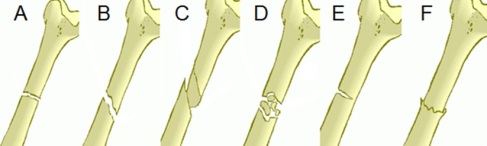
Another example of an easily identifiable disease is tuberculosis (TB), TB can cause devastating bone damage. A recent archaeological study by Lewis (2011) looked into a population who suffered from TB. Lewis visually analysed the skeletal remains of a juvenile population from Poundbury Camp, Dorset. The TB infection caused numerous ailments to the infected, such as fever, but it’s the skeletal damage which gave the indication that the person suffered. Amongst the population there was a high instance of skeletons with necrosis and lytic lesions characterised by minimal bone formation. Many of the juvenile’s vertebrae displayed new bone formations which could indicate the presence of a paravertebral abscess. Many of the metatarsals were also displaying evidence of new bone formation which they concluded could be indicative of tuberculous dactylitis. Osteomyelitis, infection of the bone, was also found on a few mandibles and visually diagnosed due to its characteristic small pores found in a localised area. It is this characterised skeletal damage, seen on numerous cases during known TB outbreaks, which cause more diseases to be easily identified by eye due to the skeletal anomalies.
There are problems when trying to differentiate certain diseases for example; TB with brucellosis (undulant fever). As they both produce spinal lesions it is necessary to observe the other characteristic skeletal damage (new bone formation and osteomyelitis) to correctly identify it as a TB infection. Another slight difference between TB and brucellosis is that the spinal lesions are more sclerotic and regular than those from a TB infection (Lewis, 2011).
These porous bones and unexpected bone formations are easily observed, as they are not what’s expected during the known skeletal development found in healthy persons. Problems arise with diseases that do no damage to the skeleton, but instead affect soft tissue and muscles. These illnesses are harder to identify as they decay over time leaving only trace elements in the surrounding soils which would then hold the key for disease identification.
References:
Hershkovitz, I. Rothschild, B. et al. 1997. Recognition of sickle cell anemia in skeletal remains of children. American Journal of Physical Anthropology. Volume 104, Issue 2. 213-226.
Lewis, M. 2011. Tuberculosis in the non-adults from Romano-British Poundbury Camp, Dorset, England. International Journal of Paleopathology. Volume 1, Issue 1. 12-23.
To learn how archaeologists and anthropologists use teeth to age skeletal remains, read our Quick Tips: How To Estimate The Chronological Age of a Human Skeleton – Using Dentition to Age Subadults. Or to read more of our interesting Quick Tips, click here.